- Panels
Try Simplicity Panel™ today by requesting a physical demo box to be mailed to your lab.

- Collection
________________________________________

Molecular Designs offers an innovative Opti-Swab Liquid Amies Transport System. This advanced solution enables reliable collection and transport of a wide range of viral and bacterial pathogens, making it suitable for various testing applications.
State-of-the-art nylon flocked nasopharyngeal and oropharyngeal swabs designed with improvements to specimen collection and diagnostic reliability in mind.

.png?width=200&height=200&name=Scribble%20(14).png)
- Extraction
A novel nucleic acid extraction system that leverages magnetic bead technology to automate the extraction process. This innovative solution lets labs perform extractions faster, at a lower cost, and more accurately.
Discover Now
Extractionless vs. Automated Extraction
Extractionless Whitepaper
Competitor Comparison
- LIS
- Resources
- About Us
- Life Science Products
- Contact Us
- Blog
Reducing the burdens of antibiotic resistant infections
.jpg)
Contents
Highlights:
-
Antibiotic resistance is costly in terms of both patient health and excess healthcare spending.
-
Molecular PCR testing combines the speed and precision necessary to identify the potential for antibiotic resistance in bacteria and allow for appropriate, timely treatment.
-
Antibiotic Resistance Add-Ons for Simplicity Panels™ (RUO) allow simultaneous pathogen and resistance marker detection for fast time to result.
Healthcare facilities and patients pay a price for antibiotic resistant infections
The costs associated with antibiotic resistant bacterial infections are going up, both for patients and for society in general. There are more than 2.8 million antibiotic resistant infections (ARIs) annually in the United States alone, resulting in 35,000 deaths and the problem is getting worse.1 A recent report by the United Nations Environment Programme estimates that, by 2050, up to 10 million deaths per year may be caused by antibiotic resistant microorganisms—a figure that is on par with current annual deaths from cancer.2 The direct and indirect costs of antibiotic resistance may soon reduce global GDP by $3.4 trillion annually and could push 24 million people into extreme poverty.2
Financial impacts of this growing problem will be felt by both healthcare facilities and patients. Costs to patients can be measured in higher healthcare bills or as increased morbidity and mortality that increase with a failure to rapidly address resistant infections. For each day an antibiotic resistant infection (ARI) is not diagnosed or effectively treated, the estimated cost of hospitalization rises by US $750.4 Failure to provide timely, targeted treatment for antibiotic resistant infections also increases the rate of re-admission, which may lead to reduced payments from Medicare and Medicaid.4,5.
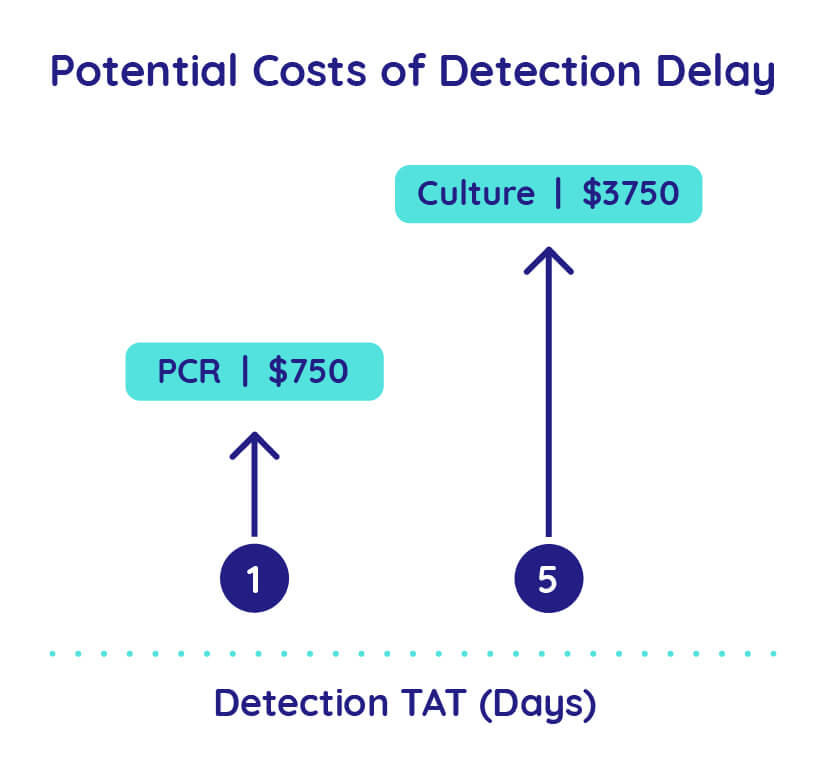
Hospitalization cost savings from reduced turnaround time of detecting antibiotic resistance markers by PCR in 1 day ($750) versus bacterial culture in 5 days ($3750).
Rapid treatment decisions can reduce costs
Three practices can reduce healthcare costs associated with antibiotic resistant infections: improved disinfection, antibiotic stewardship, and fast, precise testing.6 Traditional culture-based testing of antibiotic resistant infections typically occurs in two phases. The first 1-3 days of culture is required to isolate a bacterial pathogen. An additional 1-3 days are needed to determine which antibiotic resistances are harbored by the pathogen.7
With culture, it can take up to a week for a physician to receive test results, delaying their ability to prescribe targeted antibiotics. In an effort to treat the infection, physicians often prescribe broad-spectrum antibiotics which may prove to be ineffective if the infection is resistant to that class of drug. Delays in targeted treatment could cost the healthcare system an estimated $16,937 per patient and potentially lead to poor outcomes.8
Fast and precise testing enables rapid treatment
Molecular detection by PCR combines the speed and precision necessary to identify antibiotic resistance. With PCR, bacterial culture is not required. Instead, organisms are detected using the bacterial nucleic acids (DNA or RNA) directly obtained from a patient sample. PCR testing takes hours rather than days.
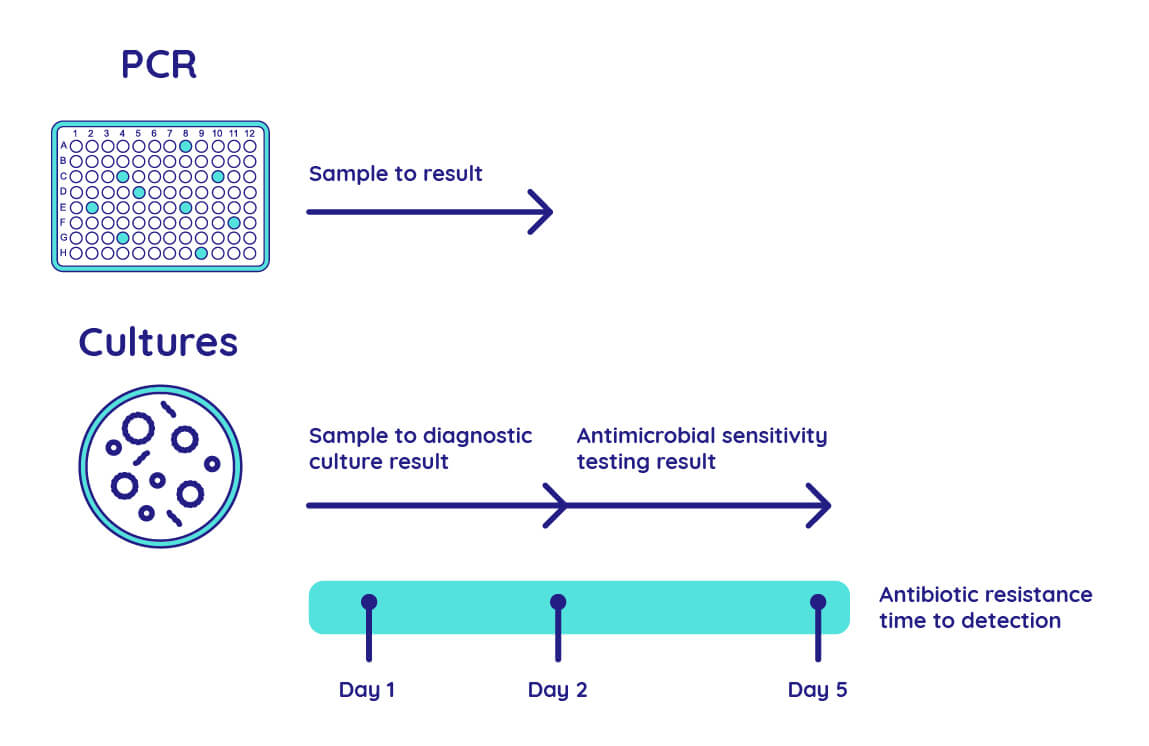
A timeline comparison between PCR and culture detection of antibiotic resistance. PCR provides single-day turnaround, while culture requires two steps (initial pathogen culture followed by antimicrobial sensitivity testing,) each of which require 1-3 days.
PCR can detect antibiotic resistance markers and pathogen-specific genes simultaneously. While antibiotic sensitivity is not identified by PCR, the detection of specific resistance markers may indicate a potential resistance to a specific class of antibiotic. This information may be used to order antimicrobial sensitivity assays to identify an effective antibiotic.
A fast, accurate identification of antibiotic resistance is important for the health and recovery of the patient, to prevent organism spread within the healthcare facility, and to reduce the prevalence of antibiotic resistant pathogens in the population. Antibiotic resistance markers on PCR panels expedite resistance detection and healthcare decision-making. By identifying targeted therapies earlier, hospitalization costs may be reduced, patients may recover faster, readmission rates may drop, and the efforts to improve antibiotic stewardship may be strengthened.
Molecular Designs Simplicity Panels™ (RUO)
Antibiotic Resistance Add-Ons for Simplicity Panels (RUO) detect resistance genes using PCR, either independently or paired with pathogen detection. By combining pathogen and antibiotic resistance targets, a single panel can distinguish bacterial from viral infections, and simultaneously report the detection of resistance markers.
| Antibiotic resistance Add-Ons for Simplicity Panels (RUO) | |
| Resistance Assay (target gene) | Associated Pathogen |
| Class A β-lactamase (blaKPC) | K. pneumoniae |
| Class A β-lactamase (CTX-M-Group 1) | Enterobacterales |
| Class B metallo-β-lactamase (blaNDM) | Enterobacterales |
| Fluoroquinolones (QNR) | Enterobacterales |
| Methicillin/Oxacillin (mecA) | Staphylococcus |
| Sulfonamides (SUL) | E. coli |
| Trimethoprim (DFR) | E. coli |
| Vancomycin (vanA, vanB) | Enterococci |
Molecular Designs offers Simplicity Panels (RUO) for an array of infectious disease organisms, including a new GI panel targeting 16 organisms associated with GI tract infections. All panels are offered in 96-well or 384-well PCR plates, and some are offered in large tube format. They have been optimized for the most common real-time PCR instrumentation.
Simplicity Panels (RUO) reduce costs with pre-plated PCR reactions. Complete reaction mixes are dispensed into the wells of the PCR plates, eliminating most liquid handling steps, minimizing reagent loss, and expediting workflows. Ninety-six-well breakaway PCR plates reduce reagent waste by allowing small to mid-sized PCR laboratories to run only the necessary reactions, with no wasted panels. This allows reference and other clinical labs to promote good antibiotic stewardship while maintaining laboratory profitability and turnaround time.
Click below to learn more about our wide selection of panels and Antibiotic Resistance Add-Ons.
Simplicity Panels™ are manufactured by Molecular Designs to GMP and ISO 13485:2016 standards. With the exception of the COVID-19 EUA, all products are for research use only and not for use in diagnostic procedures.
General Guidelines Laboratory test results should always be considered in the context of clinical observations and epidemiological data (such as local prevalence rates and current outbreak/epicenter locations) in making a final diagnosis and patient management decisions. With any test, the possibility of false-positive and false-negative results should always be considered, and the impact on patient management decisions and clinical outcomes should be carefully weighed.
References:
- Antibiotic resistance threats in the United States, 2019. (2019) doi:10.15620/cdc:82532.
- UNEP. Bracing for Superbugs: Strengthening environmental action in the One Health response to antimicrobial resistance . (2023).
- Thorpe, K. E., Joski, P. & Johnston, K. J. Antibiotic-Resistant Infection Treatment Costs Have Doubled Since 2002, Now Exceeding $2 Billion Annually. Health Aff 37, 662–669 (2018).
- Zilberberg, M. D., Nathanson, B. H., Sulham, K., Fan, W. & Shorr, A. F. 30-day readmission, antibiotics costs and costs of delay to adequate treatment of Enterobacteriaceae UTI, pneumonia, and sepsis: a retrospective cohort study. Antimicrob Resist Infect Control 6, 124 (2017).
- Hospital Readmissions Reduction Program (HRRP). Centers for Medicare & Medicaid Services. https://www.cms.gov/medicare/medicare-fee-for-service-payment/acuteinpatientpps/readmissions-reduction-program (2023).
- Avershina, E., Shapovalova, V. & Shipulin, G. Fighting Antibiotic Resistance in Hospital-Acquired Infections: Current State and Emerging Technologies in Disease Prevention, Diagnostics and Therapy. Front Microbiol 12, (2021).
- Tetz, G. & Tetz, V. Overcoming Antibiotic Resistance with Novel Paradigms of Antibiotic Selection. Microorganisms 10, 2383 (2022).
- Frédéric Michas. Average cost of inpatient day at U.S. hospitals in 2021, by hospital type . Statista https://www.statista.com/statistics/630443/inpatient-day-hospital-costs-in-us-by-nonprofit-or-profit/ (2023).


